It’s well-known that decentralized facilities like ambulatory surgical centers (ASC) can be less expensive to build and operate than traditional hospital-based surgery while building strong positive experiences and relationships with the patients in the surrounding community.
What isn’t obvious is the role these specialized facilities have already played to foster a greater sense of safety to prospective patients during the coronavirus pandemic. ASC patients intuitively believe that since ASC’s do not treat contagious patients (while hospitals do), that the ASC is a less risky environment than a hospital-based surgical suite.
Pre-existing circumstances
The popularity of the ambulatory surgical center model has ebbed and flowed for years.
The facilities often feature less restrictive building codes as well as simpler staffing models and design plans. Typically, ambulatory surgical centers charge less for identical surgical services and can offer more flexible scheduling options than inpatient surgical services.
By avoiding the most complex cases and patients with significant comorbidities, ASCs avoid high-risk patients resulting in reduced infection rates compared to hospital-based surgery. This is partly because it’s easier to prep, perform and treat a comparatively narrow variety of procedures performed within the ASC over its hospital-based counterpart/competitor.
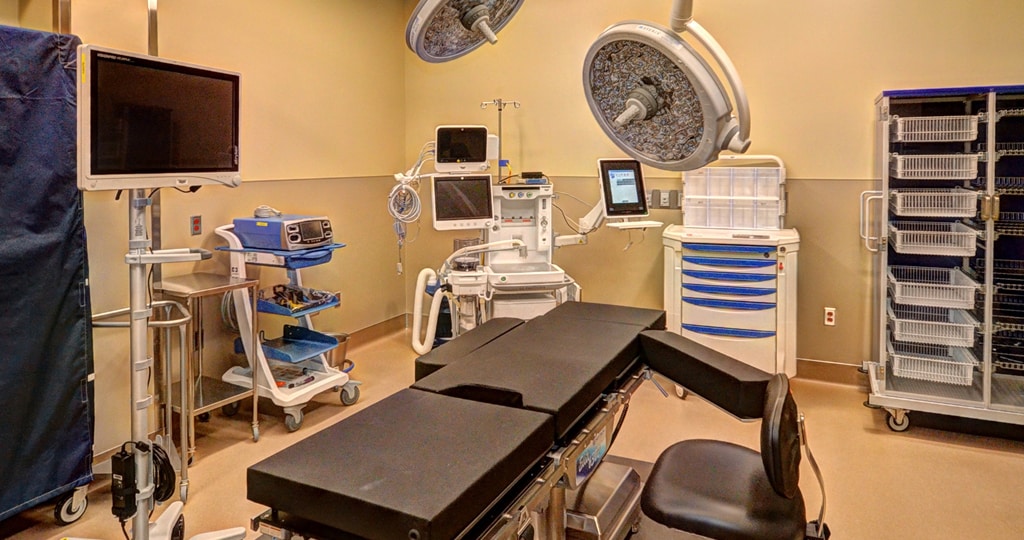
Ambulatory surgical centers have received financial incentives (even before the pandemic) as third-party payers including Medicare, Medicaid and insurance companies realized that charges for basic outpatient surgical services were often less in an ASC than in an in-hospital surgical suite.
ASCs don’t hold patients for days of monitoring, so they need not invest in on-call services, meal services or inpatient lodging. The flexibility of their service model allows ASC leaders to repurpose vacant buildings like former shopping malls or build under less demanding codes that are required by traditional hospitals where patients remain overnight.
They can also be constructed far cheaper than major hospitals because they require less space and don’t need to be centrally located within cities where real estate is more expensive. They also don’t require the full breadth of specialized equipment, facilities and staff inherent to a more centrally located catch-all hospital.
Contractors in rural areas can often make use of preassembled components that reduce construction timelines and costs by avoiding specialty tradesmen often not readily available in these locations.
Small ASCs can be located on land parcels that are highly visible but do not require larger footprints or outsized parking lots or structures that inpatient hospitals require.
The cheaper the construction cost, and the faster construction can be completed, the faster an ASC can take advantage of today’s fertile market and make a return on its investment.
Rethinking care around COVID
When COVID hit, getting a procedure done at a hospital was suddenly impossible.
Hospitals shut down anything but emergency surgery. Conversely, patients were still able to get simple surgical procedures performed in an ASC that avoided the infection potential inherent in hospitals treating COVID patients.
Important surgeries and procedures were put off during the early months of the pandemic. Many patients were in great need of services by the time ambulatory surgical centers reopened.
As major hospital systems flooded with patients suffering from COVID-19, those seeking unrelated procedures found a sense of respite in the relative safety of ambulatory surgery centers that didn’t treat COVID patients.
This phenomenon allowed inpatient hospitals to place more focus on patients with COVID-19 during the peak periods of pandemic-related treatment.
Today, it is recognized that the vast majority of surgeries do not require overnight hospital stays for patients who otherwise do not have significant health issues.
However, for all the benefits they provided, surgical centers still faced many of the same logistical challenges as places like restaurants and retail stores. There were staffing shortages, scheduling challenges and mandatory capacity limitations. And as with major hospitals, they had to increase protective equipment availability and storage and consider air exchange and filtration system improvements like negative-pressure rooms.
Fortunately, it’s far easier to modify and update smaller ambulatory surgery centers than a major inpatient hospital treating patients overnight.
Ambulatory surgery center campuses increase safety and convenience
With all of the advantages ambulatory surgery centers offer medical providers and patients, what if various outpatient services were brought together on a shared campus?
The future of healthcare campuses could take many cues from the retail industry, with several forms of medical care offered in smaller structures that share common parking, much like how retail stores cluster in shopping plazas. This could greatly reduce contact between patients.
Many private orthopedic groups have constructed ASCs that also feature orthopedic offices, physical therapy and imaging services in the same location to simplify patient treatment and follow ups.
These campuses can be easily localized within communities to emphasize high visibility and greater patient convenience.
The rising tide of ASCs and telehealth
As ambulatory surgical centers showed their value over the duration of the pandemic, another healthcare innovation has matured to help make healthcare more convenient and patients feel even safer.
Patients can use telehealth services from home to consult with their primary care provider, who can then order tests at the nearest outpatient clinic campus and make referrals to the appropriate surgical specialties. Within ambulatory clinic clusters, multiple services are easily accessible within one location for patients requiring imaging, surgical operations or physical rehabilitation.
As the medical industry and patients widely embrace a more local model of care, traditional hospital facilities stand to benefit as well.
Will the long-standing inpatient acute hospital model shed inpatient beds previously utilized for post-surgical patients as a result of the shift to ASC’s? Will this shift free facility leaders to plan for more flexible uses of their existing spaces as their patient loads ease?
Many hospital planners believe so — and we do, too.

The need for massive waiting spaces and hospital complexes that offer everything to everyone may end as more patients and medical providers embrace outpatient ambulatory surgery in tandem with the positive disruption of telehealth.
Be prepared whatever the future holds
Thanks to the pandemic, the dust got kicked up on the medical community in unexpected ways. And it has yet to settle.
Time will tell if the demand for ambulatory surgical centers will continue to accelerate. In the complex world of seemingly ever-changing reimbursement models for patient care, ASCs will likely flourish.
But medical providers need to be ready for anything.
Twenty-plus years ago, reimbursement began to favor outpatient ambulatory surgery. As hospitals lost volume to decentralized providers, Medicare altered reimbursement to favor hospital-based outpatient surgery over ASCs in a well-meaning effort to prevent hospital failures. But if hospitals are left with only the most complex patients for surgery, the cost to care for those patients may become prohibitive in these facilities’ efforts to recoup expenses previously covered by more profitable outpatient care.
A strong partnership with an experienced healthcare Design-Build firm can allow both hospitals and ambulatory surgery centers to explore their options under a variety of reimbursement scenarios.
As designers and builders of traditional hospitals and ambulatory surgical facilities alike, The Korte Company has had a finger on the pulse of this industry for six decades. Healthcare leaders rely on that experience to ensure they’ll have a solid design and construction plan in place whatever the future may bring.
Healthcare organizations must be responsive to the needs of the communities they serve. Collaborating with an experienced healthcare Design-Builder will help leaders identify how the built environment can best meet those needs. Contact The Korte Company to learn more.
